Barbara Davies RN, PhD & Nancy Edwards MSc, PhD
University of Ottawa School of Nursing
Download: Presentation (PDF, 226KB)
Learning Objectives
- Define sustainability
- Increase awareness of models about sustainability
- Increase understanding of why sustainability planning is rarely addressed in research
- Analyze facilitators and barriers to consider in developing a sustainability action plan
- Understand change and adaptation processes and why sustainability is difficult to predict
- Describe the importance of assessing the degree of sustainability using monitoring systems and data feedback mechanisms
What is Sustainability?
The degree to which an innovation continues to be used after initial efforts to secure adoption is completed
When new ways of working and improved outcomes become the norm
Sustainability is Non-linear
Multiple determinants interact at variable rates depending on contextual factors
- receptivity to new knowledge
- capacity to interpret and apply the new knowledge
- individual, organization, system levels
Model of Sustainability
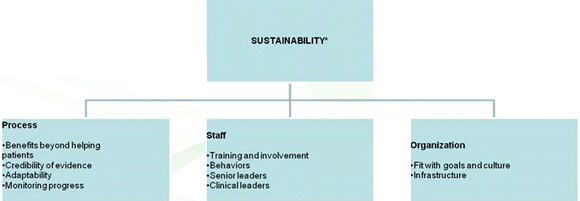
Maher, Gustafson & Evans, 2007
Why is Sustainability Planning Rarely Addressed?
- Only 2 of 1000 sources screened for a literature review about the diffusion of innovations in health service organisations included he term sustainability (Greenhalgh et al., 2005)
-
Shorter-term perspectives are the focus of health services research, possibly due to:
- Limited availability of long-term funding
- Different time perspectives of policy cycles across health care sectors
- Disengagement of project leaders towards the end of projects
Scaling Up
-
Addressing sustainability requires planning for “scaling up” knowledge use, including the following critical conditions:
- Adequate human capacity
- Supportive financial, organizational, governance, and regulatory structures
-
Issue of “boutique Interventions” designed for a specific setting but not feasible or applicable in a large scale due to resources or relevance
(Simmons et al., 2006; Hanson et al., 2003)
Factors to Consider in the Development of a Sustainability Action Plan*
The same factors can both facilitate and inhibit sustainability
(Wakerman et al., 2005):
- Relevance of the topic: Is there a well-defined need and priority for the knowledge that is being implemented? Is there consensus about what knowledge needs to be sustained and what is needed to create conditions for sustainability? How does the new knowledge fit with current priorities?
- Benefits: What are the anticipated outcomes of knowledge implementation from a biological, economic, psychological, organizational, social, political, or other perspective? How meaningful are these benefits to the various stakeholders?
- Attitudes: What are the attitudes of the patient/client, their family, the public, health care providers, and relevant decision-makers toward the innovation?
- Networks: What team or groups can be engaged to facilitate the sustainability of knowledge use? Are there people who can be engaged to cross disciplines, settings, or sectors of the health care system
- Leadership: What actions might leaders and managers at all levels of involvement take to support the sustainability of knowledge use? Are there champions for the change? Who is responsible for continued implementation of the innovation and making modifications as new knowledge is brought forward? Who will be responsible for ensuring that relevant outcomes are met?
- Policy articulation and integration: How will the fit between new knowledge and existing policies be assessed? How might the knowledge be integrated in relevant policies, procedures, regulatory and documentation systems?
- Financial: What funding is required to implement, sustain, and scale up knowledge? What flexibility in funding is necessary and available for reimbursement? Can cost-effective strategies be used?
- Political: Who are the stakeholders and what power or support might be leveraged? Who will initiate scaling up processes?
(Buchanan et al., 2007 Davies et al., 2006; Lomas; Maher et al., 2007; Nolan et al., 2005; Shediac-Rizkallah & Bone, 1998; Sibthorpe & Glasgow, 2005)
Adaptation and Why Sustainability is Difficult to Predict
The complex adaptive systems theory
(Sibthorpe, Glascow & Wells, 2005; Gunderson & Holling 2002)
- There are continuous dynamic change processes at work within each level of the health care system
- Over time, change processes at one system level may lead to change processes at the next system level
- Vertical social connections facilitate synergistic and multilevel adaptation processes
-
Factors that tend to maintain the status quo
(Gunderson & Holling, 2002; Denis & Langley, 2001):- Power hierarchies among professional groups
- Institutional routines
- Established governance structures
Monitoring Sustainability
Monitoring systems and data feedback mechanisms are needed to determine relevant process and outcome factors to assess sustainability (Pluye et al., 2004)
Four Degrees of Sustainability:
- Absent
- Precarious
- Weak
- Routinization
Future Research
-
Sustainability is a complex construct
- Participatory research designs and qualitative studies about process factors will be helpful to better understand sustainability and its determinants
-
Sustainability is a critical element of studies examining the impact of knowledge implementation for individuals, populations and the health care system
- Plans for examining sustainability required at outset of studies
- Rigorous methodology including measurement instruments is required
References
- Buchanan D.A., Fitzgerald L., Ketley, D. The Sustainability and Spread of Organizational Change. New York: Routledge; 2007: xxiii.
- Davies, B., Edwards, N., Ploeg J., Virani, T., Skelly J., Dobbins M. Determinants of the sustained use of research evidence in nursing: final report. Canadian Health Services Research Foundation & Canadian Institutes for Health Research. Ottawa, Ontario, Canada; 2006.
- Greenhalgh T., Robert G., Bate P., MacFarlane F., Kryiakidou, O. Diffusion of Innovations in Health Service Organizations: A Systematic Literature Review. Boston: Blackwell Publishing; 2005.
- Gunderson L.H., Holling C.S., Panarchy: Understanding Transformations in Human and Natural Systems. Washington, DC: Island Press; 2002.
- Hanson K., Ranson M.K., Oliveira-Cruz V., Mills A. Expanding access to priority health interventions: a framework for understanding the constraints to scaling up. Journal of Epidemiol 2002; 12[3]: 151-6.
- Maher L., Gustafson, D., Evans, A. Sustainability model and guide. NHS Institute for Innovation and Improvement; 2007.
- Mancini J.A., Marek L. Sustaining community-based programs for families: conceptualization and measurement. Family Relations 2004;53[4]: 339-47.
- NHS Institute for Innovation and Improvement. Improvement Leader’s Guide to Sustainability and Its Relationship with Spread and Adoption. 2007.
- Nolan K., Schall M.W., Erb F., Nolan T. Using a framework for spread: the case of patient access in the veterans health administration. Jt Comm J Qual Patient Saf 2005;31 [6]: 339-47
- Pluye P., Potvin L., Denis JL., Pelletier J. Program sustainability: focus on organization routines. Health Promotion Int 2004; 19[4]: 489-500.
- Rogers E.M., Diffusion of Innovations. 5th ed. New York: Free Press; 2005;429.
- Shediac-Rizkallah M.C., Bone L.R. Planning for the sustainability of community-based health programs: conceptual frameworks and future directions for research, practice and policy. Health Educ Res 1998;3 [1]: 87-108.
- Sibthorpe B.M., Glasgow N.J., Wells R.W. Emergent themes in the sustainability of primary health care innovation. MJA 2005; 183[10 Suppl]: S77-S80, page S79.
- Simmons R, Fajans P, Ghiron L. (eds.). Scaling up health service delivery: from pilot innovations to policies and programmes. WHO World Health Report; 2006.
- Wakerman J., Chalmers E.M., Humphreys J.S., Clarence C.L., Bell, A.I., Larson, A. et al. Sustainable chronic disease management in remote Australia. MJA 2005; 183 [10]: S64-S68.

